
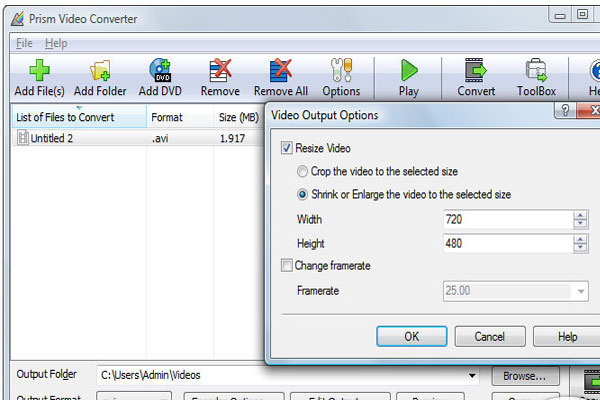
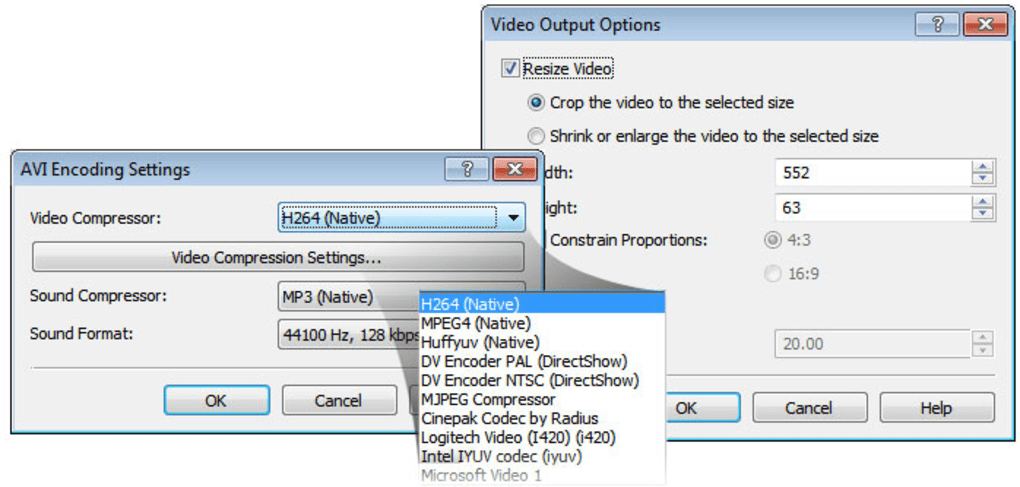
Postoperative bleeding was significantly more common in the conventional EP group than in the novel EP group (0 vs 20.75%, P = 0.028). To further reveal the safety and effect of the novel procedure, we compared the rate of adverse events, as listed in Table Table3. N group: Novel group C group: Conventional group WBC: White blood count C-RP: C-reactive protein AMY: Serum amylase LPS: Serum lipase. If the lesion was large, edge cutting could be performed before snaring argon plasma coagulation was used for bleeding (4) A guidewire was used to superselect the bile duct (BD), and the guidewire was retained in the BD (5) Electric coagulation forceps and argon plasma coagulation were used for wound hemostasis, and then the wound was closed with metal clips (6) A BD stent was implanted (7) Fibrin glue (S201110020 Bioseal, Guangzhou, China) was sprayed on the closed wound (8) Exhaust air in the stomach and stent placement were checked under X-ray and (9) The sample was sent for pathology.ġ P ≤ 0.05. The standard procedure for novel EP was as follows (Figure (Figure1, 1, Video 1): (1) The patient was placed in a supine position under general anesthesia (2) Duodenoscopy (TJF-240/TJF-260V Olympus, Tokyo, Japan) was used to observe the papillary lesion (3) A submucosal injection was performed to lift the lesion, or an injection was not performed then, en bloc or blocking resection of the lesion was performed with an endoloop (SD-7P-1/SD-221L-25 Olympus, Tokyo, Japan). As a retrospective observational study, the study was not blindly randomized. Sample size calculation with the adverse event rates of two groups (significance level of 5% and power of 80%) suggested a minimum sample size of 70.
A total of 76 patients, of whom 23 underwent novel EP and 53 underwent conventional EP, were enrolled in this study. We retrospectively studied patients who had PA and underwent novel or conventional EP at the endoscopy center of Chinese PLA General Hospital from January 2016 to September 2018.
To verify the safety and feasibility of this novel method, we reviewed the outcomes of patients undergoing novel or conventional EP. To decrease the postoperative adverse event rate of EP and improve patients’ postoperative condition, we modified conventional endoscopic papillectomy and initiated a novel procedure for endoscopic papillectomy in 2016. Thus, a better standard procedure of EP with fewer adverse events is urgently needed for the endoscopic treatment of papillary lesions. Although this is not common, it does limit the wide application of EP. These adverse events could lead to extremely difficult results that require invasive surgical intervention or even result in death. These included bleeding, operation-related pancreatitis, perforation, cholangitis, and papillary stricture, and some events, especially bleeding and perforation, are critical and even fatal. With all of these aforementioned advantages, EP seemed to be a promising treatment for PA however, surgeons also found intraoperative and postoperative adverse events. Pancreaticoduodenectomy and endoscopic papillectomy (EP) are the main treatments for PA, and EP is more recommended for benign papillary lesions because of its advantages over open surgery, including less trauma, satisfying treatment outcomes, fewer adverse events, and lower cost. Thus, the treatment of PA is essential and more critical than just follow-up. Although the main pathologic diagnosis, papillary adenoma (PA), is benign, it can potentially develop into adenocarcinoma through the adenoma-adenocarcinoma sequence. Tumors of the main duodenal papilla are rare, with a prevalence of only 0.04% to 0.12% in autopsy studies.
